05 Feb Anti-Seizure Medications Explained
TL;DR – There are multiple types of seizures and anti-seizure medications (ASMs) used to manage epilepsy. Each category of ASMs addresses seizure activity in a slightly different manner. The ASMs prescribed will vary from person to person and depend on the type of seizure that person is experiencing. It is important to consult with a healthcare provider to find the most appropriate management plan for the seizures an individual is experiencing.
Introduction
Seizures are sudden, uncontrolled electrical disturbances in the brain. Seizures can happen to anyone, but epilepsy describes conditions in which a person has an ongoing risk of seizures.
Seizures are one of the first symptoms of SLC13A5 Epilepsy. This article will review different types of seizures and the classes of medications available for patients with seizures.
I know just how overwhelming it can be to have dozens of medications listed off by a neurologist in a single appointment, and how confusing it can get. I hope this article can act as a crash course or as a reminder of what these different classes of medications are so that after you get out of that neurology appointment where the doctor recommends three new medications, you have a place to come get a simple breakdown of what those medications do. Having this article would have been so helpful when I was going through my own treatment for seizures.
Seizure Types
First, let’s review that there are multiple types of seizures and that seizures can look different, depending on the type.
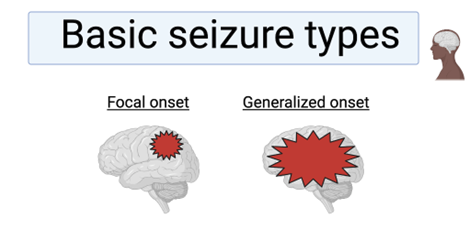
Seizures can manifest in many ways ranging from full body spasms to absent stares. Broadly, seizures are categorized based on where they start in the brain, and what changes they cause in the patient.
- Focal (Partial Seizures) start in specific brain regions, and the effects on the patient depend on the brain region: Symptoms can include muscle spasms, sensory disturbances or hallucinations, altered heart rate or breathing, or changes in emotional states.
- Generalized Seizures occur throughout the brain, and are categorized by the patient’s symptoms. Categories include:
- Absence: Loss of consciousness or responsiveness, staring into space.
- Tonic Seizures: Involuntary stiffening of muscles.
- Clonic Seizures: Involuntary jerking of muscles.
- Tonic-Clonic (formerly known as Grand-Mal) Seizures: What most people think of when they hear seizure: Stiffening and jerking of muscles, falling to the ground, loss of consciousness.
In infants with epilepsy, seizures often cause changes in heart rate or breathing; they can be subtle changes to movement or behavior, including, but not limited to: jerking of limbs or nodding of the head. Because seizures can manifest in so many ways, it can often be hard to tell what’s a seizure and what isn’t. It’s crucial to video the event and share them with your doctor. Often it is helpful to pair symptom observations with an electroencephalogram (EEG) for proper diagnosis. EEGs read the electrical activity of the brain in real time, allowing clinicians to localize the seizure and learn more about the underlying electrical disturbance between seizures.
Anti-Seizure Medications
The go-to treatment for seizures are called Anti-Seizure Medications (ASMs). The goal of these medications is to reduce and ideally control seizures. ASMs may not treat the source of the seizures, but aim to stabilize electrical activity in the brain. Each drug class works in its own unique way to prevent seizures. There are more than thirty different Anti-Seizure Medications. Many seizure medications work in multiple or even unknown ways to suppress seizures. Some of the broad categories are:
- Sodium Channel Blockers
- Calcium Channel Blockers
- Glutamate Antagonists
- GABA Enhancers: Increase inhibitory signaling
- Miscellaneous ASMs
Why are there so many types of ASMs? Each category addresses seizure activity in a slightly different manner. Before we go into how each category works, let’s review how the cells in the brain, called neurons, drive electrical activity. For more detailed information on neurons, check out our previous Science Simplified article, All About Neurons.
Excitation and Inhibition in Neurons
To understand an overactive nervous system, let’s review the basics of neuron structure and function. Neurons have a unique structure among cells, and understanding the parts can help us learn more about how they work.
- The soma, or cell body, is the control center of the neuron.
- Dendrites branch off the cell body, acting as the antenna: They “listen” for and receive messages from other neurons, which they convert into an electrical signal.
- The axon, the tail of the neuron, acts as a wire that transmits electrical signals to its target area, like a telephone wire. Axons are wrapped in myelin sheath, a fatty barrier that acts similarly to the electrical insulation around a wire.
- Once the signal reaches the axon terminals, the neuron releases specialized molecules called neurotransmitters that send a message to the dendrites of other neurons.
Generally, the signals neurons receive at their dendrites can be excitatory (increasing the neuron’s activity, a “go” signal) or inhibitory (decreasing the activity, a “stop” signal). In the brain too much excitation, or too little inhibition, can both result in uncontrolled seizure activity. So how do we rebalance the scales?
Anti-Seizure Medications: Classes and Considerations
Anti-Seizure Medications (ASMs) work by changing the balance of “go” and “stop” signals in the brain so that electrical activity doesn’t become a runaway train. We’ll now talk about specific classes of ASMs.
A note: In this section we will discuss several classes of medication: This is for informational purposes only and does not constitute medical advice. When trying medications, it is important to weigh the benefits of the drug and the cost of side effects with your healthcare provider.
Sodium Channel Blockers
Like the name suggests, sodium channel blockers work by inhibiting or blocking sodium from activating neurons, decreasing the chance of abnormal electrical activity. It is the most commonly prescribed class of Anti-Seizure Medications for a variety of focal and generalized seizures, including long-lasting seizures (status epilepticus) and childhood epilepsies.
Drugs in this class include:
- Phenytoin (Dilantin)
- Carbamazepine (Tegretol)
- Oxcarbazepine (Trileptal)
- Lamotrigine (Lamictal)
- Lacosamide (Vimpat)
- Rufinamide (Banzel)
These drugs are all prescribed as a liquid, tablet or capsule and are taken orally. Dosing is typically done based on weight and age of the patient and blood levels might be followed as well to try and tailor the dose to the needs of the patient. It is important to tell your doctor about any side effects.
Further reading:
GABA Enhancers
Gamma-Aminobutyric Acid (GABA) is an inhibitory neurotransmitter that acts like a “brake” on neuronal activity. By increasing GABA production and enhancing its effects, one can hopefully dampen activity that causes seizures. This class of drugs is used to treat generalized seizures and focal seizures. Certain drugs in this class act as “rescue” medications to quickly stop prolonged seizures (status epilepticus).
Drugs in this class include:
- Benzodiazepines
- Diazepam (Valium)
- Lorazepam (Ativan)
- Clobazam (Onfi)
- Clonazepam (Klonopin)
- Barbiturates
- Phenobarbital
- Valproic Acid
GABA Enhancers can be administered as oral, sublingual (under the tongue), or injected formulations.
Further reading:
Benzodiazepene Rescue Medications
Synaptic Vesicle Release Inhibitors
To communicate with one another at the synapse, neurons send neurotransmitters in packages called vesicles. Inhibiting the release of vesicles dampens neurotransmission, thereby decreasing the influence of neurons that are too electrically active and acting as brakes on the circuit.
Drugs in this class include:
- Levetiracetam (Keppra)
- Brivaracetam (Briviact)
Further reading:
Glutamate Antagonists
Glutamate is the most prominent excitatory neurotransmitter in the brain. Glutamate released from an axon terminal can bind to many receptors that act as “go” signals for neurons, so it has many ways of increasing overall activity. Glutamate Antagonists block these receptors, reducing excitation in the brain to manage seizures.
Drugs in this class include:
- AMPA receptor antagonists
- Perampanel
- Drugs with uncertain mechanism thought to affect glutamate receptors and other excitatory/inhibitory signals
- Topiramate
- Felbamate
Further reading:
Glutamate Antagonists: AMPA receptor inhibitors
Miscellaneous ASMs
As the name suggests, Miscellaneous ASMs are a group of epilepsy medications that do not fit into any of the above mentioned traditional categories. These medications are not typically used right away to treat epilepsy, instead they are used when traditional seizure medications have not provided sufficient control of seizures.
- Drugs in this class include:
- Ezogabine (Retigabine)
- Cannabidiol (CBD)
Each of these Miscellaneous ASMs target a different type of seizure and have their own benefits and side effects. Although they fall under the same class of medications, they each have a unique pharmacological makeup.
Some people find seizure control by taking just one ASM, while others require a combination of several. When on any of these medications it is important to be in contact with your Neurologist so they can monitor seizure frequency and help manage symptoms. For SLC13A5 Epilepsy, we are currently collecting information about the most commonly used ASMs, and which may be the most effective, as a part of our Natural History Study. Be sure to stay tuned for updates as we continue our Natural History Study!
If you want to find out more information about medications, you can review some of these resources:
https://www.epilepsy.com/stories/summary-anti-seizure-medications
https://www.myadlm.org/CLN/Articles/2013/june/Antiepileptic-Drugs
https://my.clevelandclinic.org/health/treatments/24781-antiseizure-medications-anticonvulsants
The author of this article, Kaitlyn O’Connor is a rising junior at Pitzer College. Where she is pursuing a bachelor of arts in Psychology as well as a minor in Spanish. She is passionate about helping others and hopes to one day have a career in healthcare helping kids facing medical challenges like she once did.
This article was reviewed by Dylan Verden, PhD, and Brenda Porter, MD, PhD.
Figures were created using BioRender.com.
Is there a topic you want to see covered in Science Simplified? Let us know by emailing science@tessfoundation.org.